GP Practice
Teaser text here....the Title link and Read More points to an RCCL article URLThe Skinny on Peculiar Skin
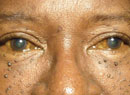
A 67-year-old black female reported to the office with a chief complaint of blurry vision at near, as well as facial skin lesions. She asked if there was any medication that could improve her skin cosmesis. Her systemic history was remarkable for hypetension, diabetes and dyslipidemia, which was well controlled medically with lisinopril, metformin and a statin, respectively.
A Stroke of Bad Luck
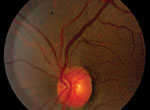
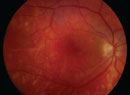
Sudden-onset, unilateral, painless vision loss is certainly a cause for patient and doctor concern as it may indicate acute retinal ischemia (ARI). Transient monocular vision loss (TMVL) is the most common symptom of ARI with an incidence of approximately 14 per 100,000. Ophthalmic exams on TMVL patients usually lack significant findings and sequelae. In contrast, ARI from artery occlusions produce permanent visual acuity, visual field loss, or both. Though treatment is mostly futile in restoring vision in these cases, patients should still be emergently referred for a stroke work-up.
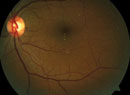
A Diagnosis for the Birds
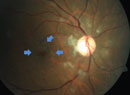
A 61-year-old Caucasian female presented with symptoms of blurred vision in both eyes for the past year and a half. She also reported seeing dark floaters in her vision that she described as having white halos surrounding them.
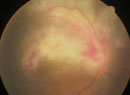
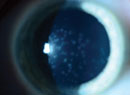
CMV: Old Foe, New Victims
CMV gained recognition during the human immunodeficiency virus (HIV)/acquired immune deficiency syndrome (AIDS) epidemic for causing infectious retinitis in susceptible patients. More recently, it has emerged as a cause of ocular and systemic sequelae in immunocompetent patients.3,4
The News Feed
Study: Eye Dominance, Acuity are Independent
Hyaluronan Regulates Limbal Lymphatic Growth
Seborrheic Dermatitis May Cause MGD, DED
High Myopia Linked to AMD Risk
New Scoring System for Keratoconus Progression
Study: Bilateral Anti-VEGF Shots OK
At Age 60, PVD Progresses Faster in Women
More Evidence Encourages Time Outdoors for Myopia
Study Ranks Contact Lens Compliance
African Americans More Likely to Have PACG
Anti-VEGF Impacts Short-term Ocular Circulation
Men at Higher Risk for Worse DME
Pre-Treatment IOP Reveals Location of Early Progression
Ocular Measurements Affected by Diurnal Course
Why Time Seems to ‘Fly By’ As We Age
Diabetic Eyes Without DR Still Have Reduced Optical Quality
Subjective Vision Matters Most to Presbyopes
Young, Elderly at Risk for Ocular Toxin Exposure
Cataract Care: Can a Carrot Replace the Scalpel?
Expanded Parameters for Daily Disposable Torics
New Antiviral Hits the Market
New Cancer Staging Criteria Predict Survival Better
Reading Drug Labels is Impossible For Emerging Presbyopes
High Calcium Intake Linked to Lower Risk of Late AMD
Older Patients Not Opposed to Telemedicine
Steroids, Other Risks Linked to CSR Development
Glaucoma Less Likely in Caucasians than Asians
Acuvue Oasys Transitions Now Available
Easier Glaucoma Analysis for Heidelberg OCT
Repeat PK Promotes Better Healing than Primary Surgery
Diabetic Children at Risk for Retinal Microvasculopathy
Reduced Choroidal Density a Glaucoma Predictor
Better Nutrition May Protect Against Amblyopia
Sleep Problems Cause Uptick in Dry Eye Cases
Avoid Diplopia-related Problems in Surgical Patients
Exfoliation Syndrome Increases Risk of COPD
Inpatient Caregivers Neglect Glaucoma Regimens
Demodex Common in Patients With Ocular Discomfort
Treatment Hiatus a Risk for DR Progression
Three Glaucoma Risk Factors Identified in CRVO Patients
Blood Pressure Predicts Visual Field Changes in NTG Eyes
Chronic SEIs Decrease Corneal Transparency
Arkansas Scope Bill Moves to Governor’s Office
Watch Out for DED in Migraine Sufferers
Don’t Skip Pediatric Oculomotor Testing
Mnemonic Helps Catch Small Choroidal Melanoma Early
IOP Spike May Mirror Sports Stress
Early Cataract Surgery a No-go for Some Infants
Contact Lens Slows Corneal Melt
Look Inside The Current Issue
Features
Anti-VEGF: Where Are We Now?
Can You Spot These Retinal Vascular Abnormalities? test
Dry Eye Drugs: New Approaches to an Old Problem
My Patient Has Glaucoma...Now What?
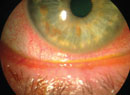
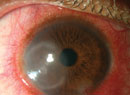
Red Eye Roundup
The Changing Landscape of Glaucoma Therapy
Departments
A Diagnosis for the Birds
A Stroke of Bad Luck
Beware the Red Herring LEMS
CMV: Old Foe, New Victims
Don’t Bet on Red
Glaucoma Tools: Know the New Codes
In Between Days
Let the Truth Set You Free
New Meds: Today and Tomorrow
RPE: The Multitasking Master
The Skinny on Peculiar Skin
Twice the Conditions, Twice the Fun
Continuing Education
Can You Spot These Retinal Vascular Abnormalities?
Take a Clinical Approach to Anterior Uveitis
Additional Publications
-
Annual Contact Lenses and Lens Care Guide-2022
Hear from several experts, including Miguel A. Busquets, MD, Carolyn Majcher, OD, and Mary Anne C. Murphy, OD, about how to manage geographic atrophy using modern-day tools, technology, treatments and knowledge.
Sponsored by Apellis Pharmaceuticals Inc and Carl Zeiss Meditec USA, Inc Clinical Perspectives on Patient Care
Digital Devices are Impacting Your Patients
Opthalmic Product Guide
Practical Matters in Myopia Management
Innovations in Glaucoma Care & Treatment
Review of Cornea & Contact Lenses
-
A Systematic Approach to Solving Contact Lens Discomfort
Comfort may be the number one factor in achieving a successful, long-lasting contact lens fit. Take a stepwise approach when comfort can’t be found. -
Ring Around the Cornea
Peripheral edema occurring many years post-op, signifying Brown-McLean syndrome, may be initially alarming, but it’s nothing to worry about. -
How to Refit the Unhappy Multifocal Patient
These tips can help you turn a negative experience into a postitive one. -
Four Contact Lens Complications to Combat
Any one of these could cause significant visual problems, so do your best to be proactive to prevent further damage. -
Get Daily Disposables On Your Radar
These lenses come with many benefits, but we need to make sure we’re doing our best to shed light on what they are. -
Navigating the Crosslinking Possibilities
Future modifications to the standard protocol already in use abroad may soon make their way stateside.

Women In Optometry continues to be published online, with regular updates on practice design, practice success, news, trends and perspectives. Visit womeninoptometry.com.